Nearly 43% of older adults with chronic conditions miss their medications regularly, yet most people still blame simple forgetfulness. That assumption is dangerously incomplete. Missing doses is a complex problem rooted in physical limitations, emotional resistance, medication complexity, and a healthcare system that often makes adherence harder than it should be. This article walks caregivers and older adults through the real causes of missed medications and offers evidence-based strategies to build a routine that actually works, even when life gets complicated.
Table of Contents
- What really causes missed medications?
- Why reminders alone don't solve the problem
- How complexity and polypharmacy increase the risk
- Practical strategies for caregivers and patients
- A new approach: Tailoring solutions beyond reminders
- How ReMoe helps you stay on track
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Missed medications have many causes | Forgetfulness is just one reason; physical, emotional, and system factors are key. |
| Polypharmacy raises risks | Taking many medications or complex regimens leads to more errors and missed doses. |
| Reminders alone aren’t enough | Technology helps but doesn’t solve nonadherence when root causes remain unaddressed. |
| Tailored strategies work best | A mix of tools, discussion, and regular reviews delivers the best adherence. |
| Caregivers play a critical role | Personal reminders and support often outperform apps for at-risk individuals. |
What really causes missed medications?
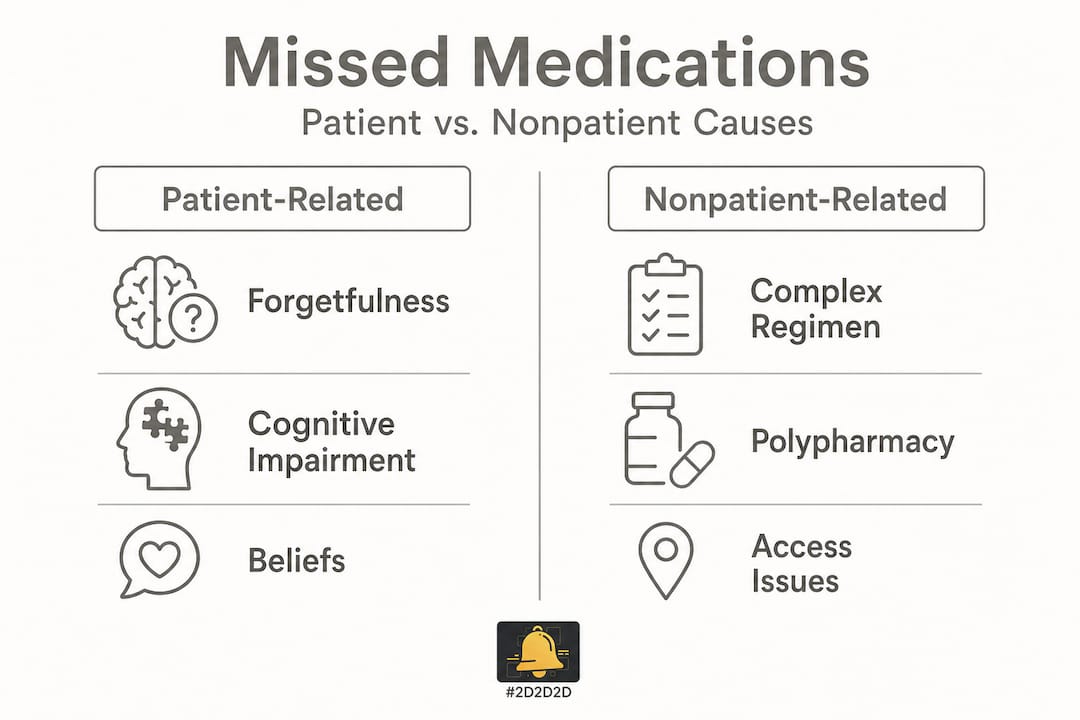
Most people picture an elderly person who simply forgot to take a pill. The reality is much more layered. Patient factors causing missed medications in elderly individuals include cognitive impairment, poor health literacy, physical limitations like dexterity issues, and deeply held beliefs about whether medications are truly necessary.
Cognitive decline is one of the most serious patient-side barriers. A person with early dementia may not remember whether they took a dose, leading to either skipping or double-dosing. Poor health literacy, meaning difficulty understanding medication labels or instructions, makes it easy to misread a schedule. Physical limitations also matter enormously. Arthritic hands may struggle to open a child-proof cap, and vision problems can make reading small print nearly impossible.
Personal beliefs play a bigger role than most caregivers realize. Some older adults believe medications are a sign of weakness, worry about dependency, or feel their body "knows best" without pills. These beliefs are rarely discussed openly at doctor's appointments, yet they directly influence daily behavior.
On the other side of the equation, nonpatient factors include polypharmacy (taking five or more medications), complex dosing regimens, high out-of-pocket costs, unpleasant side effects, multiple prescribers who don't coordinate, and poor communication from healthcare providers. When a person sees three different specialists and each one adds a medication, nobody has the full picture. That fragmentation breeds confusion.
Consider what a typical complex regimen looks like: one medication taken with food twice daily, another taken on an empty stomach once in the morning, a third taken every other day, and a fourth taken as needed for symptoms. Keeping all of that straight is a genuine cognitive challenge, even for sharp, healthy adults.
Patient vs. nonpatient causes at a glance
| Category | Factor | Example |
|---|---|---|
| Patient-related | Cognitive impairment | Forgetting whether a dose was taken |
| Patient-related | Poor health literacy | Misreading dosing instructions |
| Patient-related | Dexterity problems | Unable to open pill bottles |
| Patient-related | Personal beliefs | Thinking the medication is unnecessary |
| Nonpatient | Polypharmacy | Five or more prescriptions daily |
| Nonpatient | Complex regimen | Different timing rules for each drug |
| Nonpatient | High cost | Choosing between medication and groceries |
| Nonpatient | Multiple prescribers | Conflicting or duplicated medications |
| Nonpatient | Side effects | Nausea, dizziness, or fatigue from a drug |
Nearly 70% of U.S. adults between the ages of 40 and 79 take at least one prescription medication. A full 22% take five or more, which dramatically increases the risk of errors and missed doses. Building a strong daily habit checklist is one of the first steps caregivers can take to bring order to a complicated medication schedule.
The takeaway here is not that patients are careless. It is that the entire medication management system often works against the people who need it most.
Why reminders alone don't solve the problem
Setting a phone alarm seems like the obvious fix. It is a start, but it is far from a complete solution. The deeper issue is that some people skip medications on purpose, and no reminder can override a deliberate choice.
Intentional nonadherence is driven by emotional resistance, unpleasant side effects like nausea or dizziness, fear of dependency, and the absence of a trusted caregiver who checks in regularly. When a medication makes someone feel worse than their condition does, they stop taking it. That is a rational decision from their perspective, even if it is medically risky.
Here are the most common situations where reminders alone fail:
- Cognitive impairment. A person may hear the alarm and not understand what it means or what action to take.
- Deliberate refusal. If someone has decided they do not want to take a medication, a notification only creates frustration.
- Side effect avoidance. The reminder triggers anxiety rather than action because the person associates the pill with feeling sick.
- Lack of trust. If a patient does not trust their prescriber's reasoning, they may ignore reminders as a form of passive resistance.
- Alarm fatigue. Too many reminders from too many sources cause people to tune them all out.
"Real adherence often requires a combination of technology, personal relationships, and clinical support. No app can replace a trusted caregiver or a doctor who takes the time to truly listen."
Edge cases in medication nonadherence show that personal caregiver reminders are often more effective than technology alone. For patients who refuse medications due to side effects or dependency fears, the answer is a sensitive conversation with the prescriber. Sometimes, switching to a liquid formulation, adjusting the timing, or splitting a dose across the day resolves the resistance without abandoning the treatment entirely.
Pro Tip: If your loved one regularly "forgets" their medication right after a doctor's visit, ask them directly how the medication makes them feel. Intentional skipping often masquerades as forgetfulness, and addressing the root cause will do more than any reminder app.
Pairing personalized reminder strategies with real conversations is the most effective combination. Technology supports the process but cannot carry it alone.
How complexity and polypharmacy increase the risk
Polypharmacy is defined as the regular use of five or more medications simultaneously. It is not a fringe situation. For older adults managing conditions like diabetes, high blood pressure, heart disease, and arthritis all at once, five or more prescriptions is very common.

The numbers are striking. A meta-analysis of 51 studies found that medication nonadherence averages 43% among older adults with chronic conditions. And over half of older adults with multiple conditions and what researchers call hyperpolypharmacy, meaning ten or more medications, show low or medium adherence. The more medications a person takes, the harder it becomes to stay consistent.
Adherence rates by medication burden
| Medication count | Approximate adherence rate | Risk level |
|---|---|---|
| 1 to 2 medications | High adherence (roughly 75-85%) | Low |
| 3 to 4 medications | Moderate adherence (roughly 60-70%) | Moderate |
| 5 or more medications | Low to moderate (below 57%) | High |
| 10 or more medications | Low adherence (below 50%) | Very high |
Complex regimens are mentally exhausting. Imagine managing a drug taken with food twice a day, a second taken 30 minutes before breakfast, a third only on weekdays, and a blood thinner that requires regular lab monitoring. The mental load alone is a significant barrier, especially for older adults who may also be managing chronic pain, fatigue, or memory concerns.
Here is what actually helps reduce that burden:
- Maintain a master medication list. A single document listing every medication, the prescriber, the dose, and the timing makes reviews and emergencies easier to manage.
- Use a single pharmacy. Filling all prescriptions at one pharmacy lets the pharmacist catch dangerous interactions that individual doctors may miss.
- Request blister pack or bubble pack dispensing. Many pharmacies offer pre-sorted packs by day and time, removing the daily decision-making entirely.
- Ask about medication synchronization. This service aligns all refills to the same pickup date each month, reducing missed refills.
Pro Tip: At your next doctor's appointment, ask specifically, "Is there any medication on my list that we could stop or simplify?" Deprescribing, the intentional reduction of medications that are no longer necessary, can dramatically improve adherence and quality of life.
Using multi-reminder systems can help bridge the gap while you work on simplifying the regimen itself. Tools that organize reminders by time of day and priority reduce the cognitive effort required each day.
Practical strategies for caregivers and patients
Understanding the problem is one thing. Doing something about it is another. Here is a step-by-step action plan that caregivers and patients can start using immediately.
-
Create a complete medication inventory. List every medication, the prescribing doctor, the purpose, the dose, and the timing. Review this list at every medical appointment. Medication management strategies suggest that coordinating through a single list and regular reviews significantly reduces errors caused by multiple prescribers.
-
Consolidate prescribers where possible. Having a primary care physician serve as the central coordinator for all medications reduces the risk of duplication or dangerous combinations.
-
Use a physical pill organizer. A weekly pill organizer sorted by day and time of day removes the daily question of whether a dose was taken. The empty slot is the answer.
-
Set up layered reminders. Combine a phone alert, a calendar entry, and a caregiver check-in for the most critical medications. No single system is foolproof.
-
Track side effects in writing. Keep a simple log noting the date, the medication, and the side effect. Bring this log to every appointment. Prescribers can only adjust a regimen if they know what is happening.
-
Schedule a quarterly medication review. Every three months, ask the prescriber to look at the full medication list and identify anything that can be stopped, reduced, or simplified.
-
Build medication times into existing habits. Taking a blood pressure medication with morning coffee or an evening pill with brushing teeth links the dose to an action that already happens automatically.
Pro Tip: Document every side effect, even minor ones like mild drowsiness or a slight stomach upset. Patterns matter. What seems unrelated may turn out to be a drug interaction, and having a written record saves time and gives the doctor something concrete to work with.
Linking medication management to a broader daily adherence checklist keeps everything in one place and prevents any single task from slipping through the cracks. Combining that with using multiple reminder systems creates redundancy that protects against the inevitable bad days.
A new approach: Tailoring solutions beyond reminders
Here is what most medication guides get wrong. They present a list of tools and assume that adding the right app or the right pill organizer will solve the problem. But nonadherence persists despite these interventions because the underlying causes are too varied for any single solution to address. Lasting adherence needs a tailored, multifactorial approach.
The contrarian insight worth sitting with is this: sometimes, less is more. When a patient is overwhelmed by ten medications, adding a more sophisticated reminder system adds complexity to an already complicated life. The more powerful intervention might be asking the doctor to deprescribe two of those ten medications. A simpler regimen that gets taken consistently beats a complex one that gets partially followed.
There is also a tension in how different experts frame the problem. Some place patient beliefs and healthcare system failures at the center. Others focus on pharmacological complexity as the primary driver. Both are right, depending on the individual. A 72-year-old with strong health literacy but 12 medications faces a different challenge than a 68-year-old with early cognitive decline and only three prescriptions. Treating them the same way will not work.
The most effective approach we see combines three elements. First, technology for structure, because reminders and role-based reminders that assign tasks to caregivers or family members create accountability without placing all the burden on one person. Second, regular clinical reviews to reduce the medication burden where possible. Third, genuine human conversation that surfaces fears, side effects, and beliefs before they quietly become missed doses.
No single intervention works for everyone. The goal is not to find the perfect tool. It is to find the right combination for each individual person and adjust it over time as needs change.
How ReMoe helps you stay on track
Managing medications is not a technology problem, but the right technology makes everything easier.
Once you have thought through the strategies above, a dedicated reminder app can tie all the moving pieces together in one place. ReMoe is built around exactly that idea: your whole life organized in one place, from medication reminders to bills, schedules, and anything else that matters. With AI reminder features that adapt to your schedule, ReMoe makes it simple to set layered alerts for different medications at different times of day. Caregivers can coordinate reminders with family members so that no single person carries all the responsibility. Try ReMoe today and see how a central reminder system supports every other strategy you put in place. Plans are affordable, and you can see pricing to find the right fit for your household.
Frequently asked questions
Which patients are most at risk for missing medications?
Older adults with multiple chronic conditions and those with cognitive impairment are especially at risk, as patient factors like memory loss, poor health literacy, and physical limitations all contribute to missed doses.
How common is medication nonadherence in the elderly?
Medication nonadherence affects about 43% of older adults with chronic health conditions, according to a meta-analysis of 51 studies, making it one of the most significant issues in elderly care.
What is polypharmacy and why does it matter?
Polypharmacy means taking five or more medications regularly, and it matters because 22% of adults over 40 already take that many, which dramatically increases the chance of errors, interactions, and missed doses.
Are reminder apps enough for medication management?
Reminder apps are a helpful layer, but they cannot address all the reasons people skip medications, since intentional skipping driven by side effects, fear, or emotional resistance requires personal and medical support alongside any technology.